

The NHS prides itself on being a national institution built on public service and professional dedication. Yet beneath the surface lies a stark divide. Some hospitals have become environments where clinicians build long careers, where teams feel supported and leadership is trusted. Others have become places defined by exhaustion, high turnover and declining morale.
New workforce data reveals a widening gap between the best and worst NHS hospitals to work in England. At the top of the system, staff engagement remains high and teams report confidence in their organisations. At the bottom, the picture is far darker. In some hospitals fewer than four in ten employees say they would recommend their workplace to colleagues.
For a service already facing record waiting lists and staff shortages, the implications are significant.
A Tale of Two NHS Workplaces
Across England’s acute hospital sector, the proportion of staff who say they would recommend their organisation as a place to work has fallen to just under 57 per cent. That represents a reversal after several years of recovery and suggests workforce pressure is once again eroding morale across the service.
Yet this national average masks a striking divide. A handful of NHS organisations consistently outperform their peers, maintaining high levels of staff satisfaction even as the wider system struggles. These hospitals have developed reputations as stable, well-led workplaces where clinicians feel able to deliver safe care and build sustainable careers.
University College London Hospitals sits firmly at the top of the rankings. Nearly eight out of ten employees say they would recommend the organisation as a place to work. Guy’s and St Thomas’, Royal Berkshire and Northumbria Healthcare follow closely behind, each maintaining staff endorsement rates well above the national average.
These organisations share a number of common characteristics. Leadership teams are stable. Clinical governance structures are strong. Investment in staff wellbeing and professional development is visible rather than rhetorical. In many cases they are also large teaching hospitals connected to universities and research centres, giving clinicians opportunities to develop academically as well as clinically.
In a workforce environment where burnout has become a defining challenge, these institutions show that organisational culture still matters.
Best NHS Hospitals to Work At
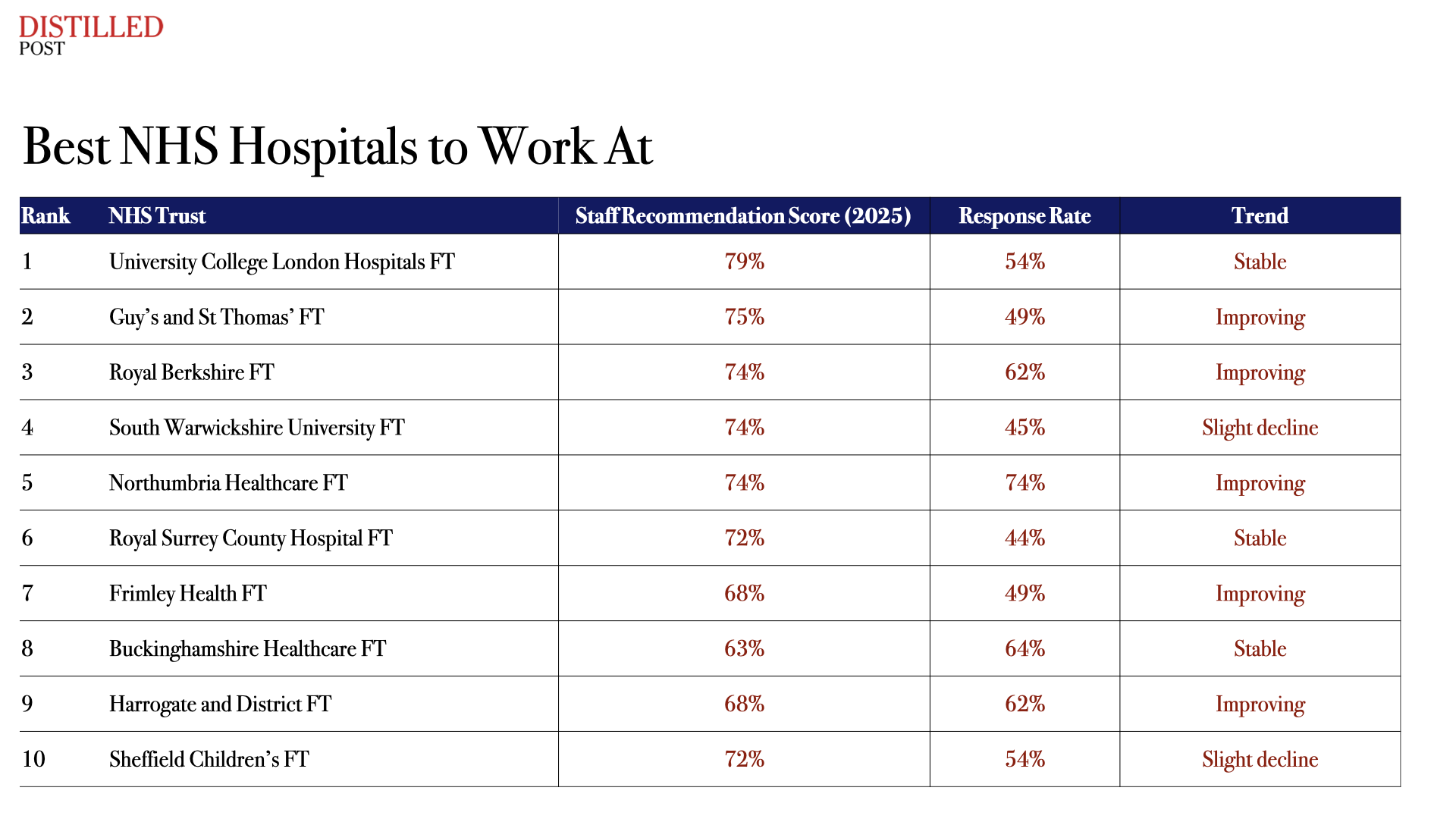
These trusts represent the upper tier of NHS employers. Staff working in these organisations consistently report strong teamwork, supportive management and better working environments.
Where the System Is Struggling
If the best trusts demonstrate what strong leadership and culture can achieve, the lowest-ranked hospitals reveal the scale of the NHS workforce challenge.
Several hospitals recorded strikingly low levels of staff recommendation. Mid and South Essex sits at the bottom of the national rankings, with only around a third of employees saying they would recommend the trust as a workplace. Close behind are the Queen Elizabeth Hospital King’s Lynn, East Kent Hospitals University and Countess of Chester Hospital.
These scores reflect more than internal dissatisfaction. They often signal deeper organisational challenges such as workforce shortages, operational instability or sustained pressure on clinical services.
In some cases the decline has been particularly sharp. Trusts such as Royal Cornwall Hospitals and Sherwood Forest Hospitals have seen dramatic drops in staff endorsement over recent years. When satisfaction falls this quickly it often indicates systemic strain rather than isolated issues.
The consequences extend well beyond staff morale. Hospitals with lower workforce engagement frequently struggle to recruit experienced clinicians. Vacancies increase. Agency staffing costs rise. Operational performance deteriorates.
Ultimately the effects are felt by patients.
Worst NHS Hospitals to Work At
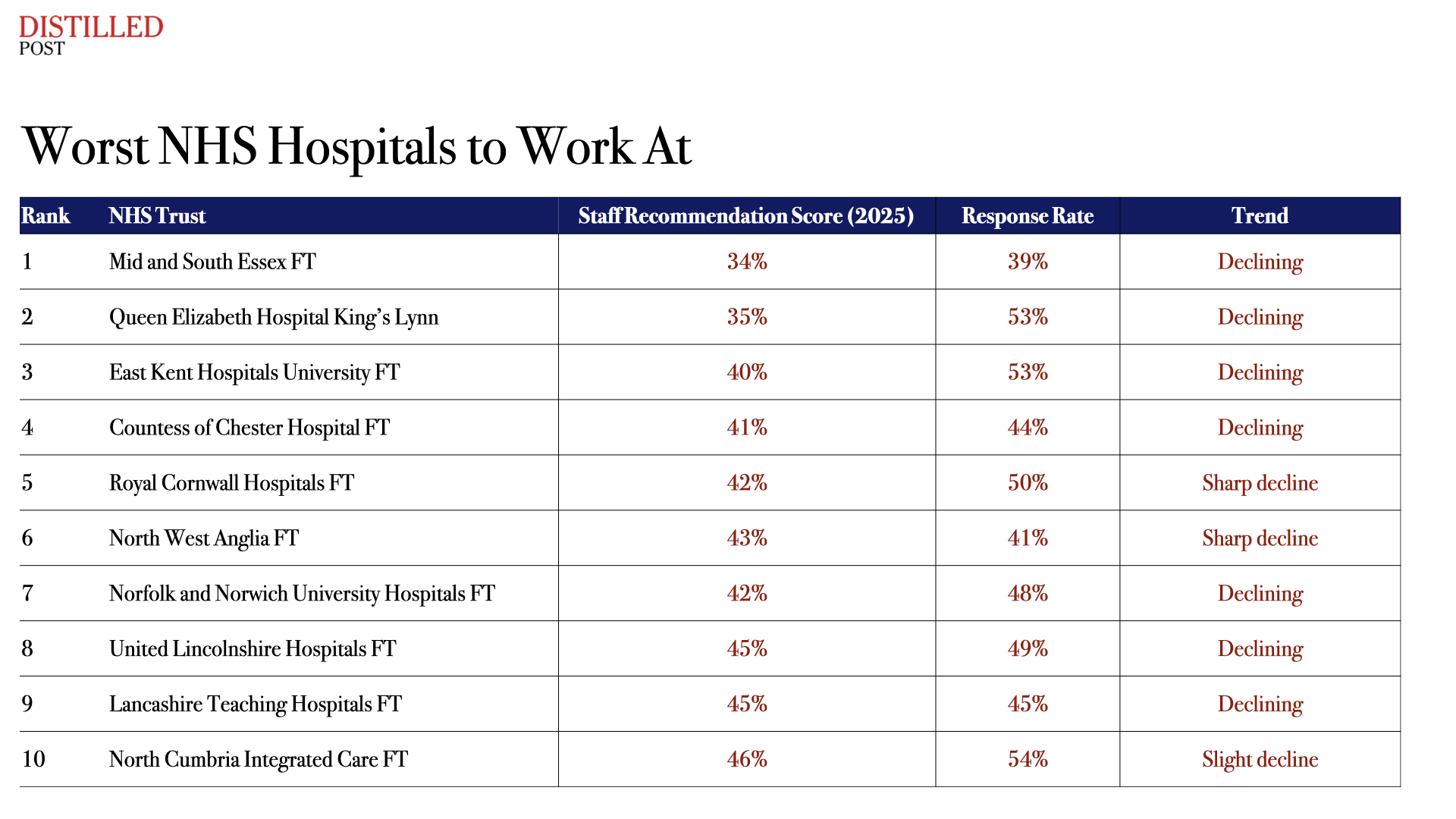
Across these organisations fewer than half of staff would recommend their hospital as a workplace.
That is a stark signal in a system that depends heavily on workforce stability.
Why the Gap Between Hospitals Is Growing
The widening divide between NHS workplaces reflects deeper structural pressures within the health service.
Workload remains the most obvious factor. Hospitals operating under extreme demand struggle to maintain safe staffing levels, increasing pressure on frontline teams. Over time that pressure becomes burnout.
Leadership stability also plays a major role. Organisations with consistent executive leadership tend to maintain stronger cultures and clearer strategic direction. Where leadership changes frequently, staff confidence often deteriorates.
Investment is another key driver. Hospitals with modern infrastructure, digital systems and well-funded clinical environments tend to reduce administrative burdens on clinicians. This improves both efficiency and staff satisfaction.
Finally there is organisational culture. Hospitals that actively prioritise staff wellbeing, mentorship and career progression often retain talent more successfully than those focused purely on operational metrics.
These forces create a powerful feedback loop.
High-performing trusts attract talented clinicians, reinforcing their performance and reputation. Struggling organisations lose experienced staff, which intensifies operational pressure and accelerates decline.
Over time the gap widens.
The Workforce Challenge Facing the NHS
For policymakers, the lesson is increasingly clear.
The NHS workforce crisis cannot be solved through recruitment alone. Hiring more doctors and nurses will help, but it will not address the deeper issues driving staff dissatisfaction.
Retention is now the defining challenge.
If clinicians feel valued, supported and able to deliver high-quality care, they stay. If they feel overwhelmed and unsupported, they leave.
The best NHS hospitals show what strong leadership and organisational culture can achieve even under pressure. The worst illustrate what happens when those foundations weaken.
For a health service built on the dedication of its workforce, the stakes could not be higher.
Because ultimately the future of the NHS will not be decided solely by funding settlements, new technology or policy reforms.
It will be decided by whether the people working inside its hospitals still believe those institutions are places worth building their careers.