

The National Health Service is approaching a critical inflection point. After years of rising waiting lists, missed performance standards and relentless political scrutiny, NHS England believes it may finally be within reach of a symbolic milestone: restoring momentum in elective care. At the centre of the effort is Sir Jim Mackey, who has overseen the national elective recovery drive since assuming responsibility for the programme in 2024. The objective is clear, reduce waiting times and demonstrate that the NHS can once again deliver timely care.
What appears to be a modest statistical improvement carries major significance for the health system and for government credibility. The NHS is aiming to bring around 65 percent of patients within the 18-week referral-to-treatment standard by the end of the financial year. For a system that has struggled for years to halt deterioration in performance, reaching that threshold would represent the first visible reversal of the pandemic-era collapse in elective care delivery.
The recovery push has been driven by what senior leaders describe as an “elective sprint”, a concentrated national effort to increase activity in the final months of the year. Approximately £120 million in additional funding has been directed toward hospitals to expand operating theatre schedules, accelerate outpatient procedures and increase diagnostic throughput. Hospitals across England have been encouraged to run extended clinics, open additional theatre lists and rapidly clear patients who can be treated quickly.
Operationally the strategy is simple: move as many patients as possible through the system in the shortest possible timeframe. The aim is not merely to reduce waiting lists but to restore confidence that the NHS can meet the expectations placed upon it. After years in which performance targets have been repeatedly missed, NHS England leadership understands that credibility now hinges on demonstrating measurable progress.
The trajectory of performance illustrates both the challenge and the progress. Throughout much of the past year the proportion of patients treated within 18 weeks remained largely stagnant, hovering close to the low-60 percent range. Only in recent months has the trend begun to edge upward, suggesting that the late-stage surge in activity may be having the intended effect.
Elective RTT Performance vs 65% Target
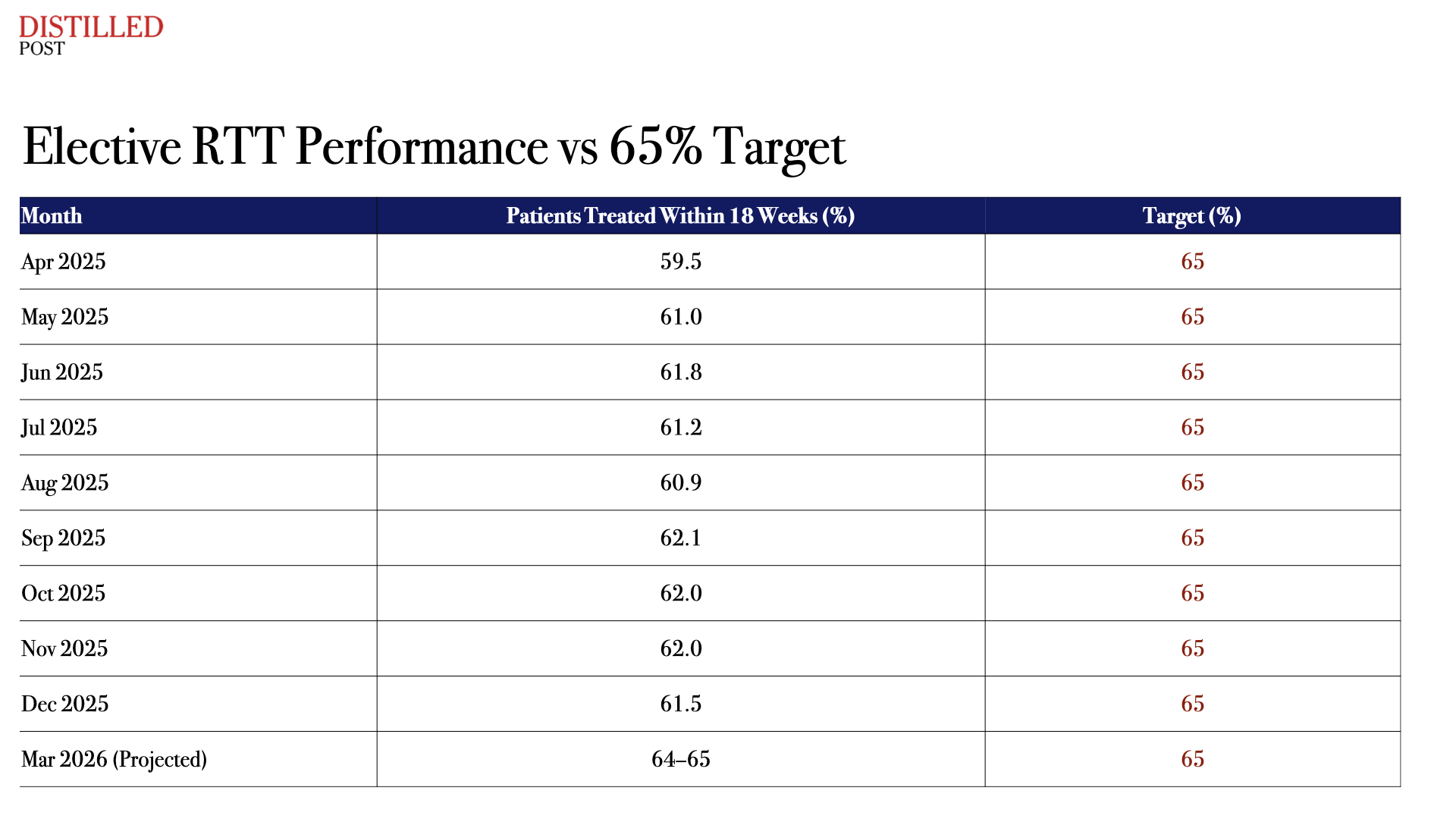
Yet the apparent progress masks a more complicated reality beneath the headline metric. Within NHS leadership circles there is growing concern that the pressure to meet a single national target may inadvertently reshape clinical priorities across the system. When hospitals are required to move patients through the pathway quickly, they inevitably prioritise procedures that can be completed efficiently.
These tend to be outpatient interventions, diagnostic investigations or routine surgeries that require limited theatre time. Complex operations, by contrast, demand far greater resources. They involve specialist surgical teams, longer operating sessions and extended hospital recovery periods. In an environment where activity is being measured weekly against a national target, the system naturally gravitates toward the quickest achievable gains.
This has raised alarms among some clinicians and operational leaders who fear that the longest-waiting patients may become invisible within the broader recovery narrative. The NHS has set a separate objective of reducing the proportion of patients waiting more than 52 weeks to below one percent of the total waiting list. Achieving that target has proven significantly more difficult.
52-Week Waiting List Breaches vs Target
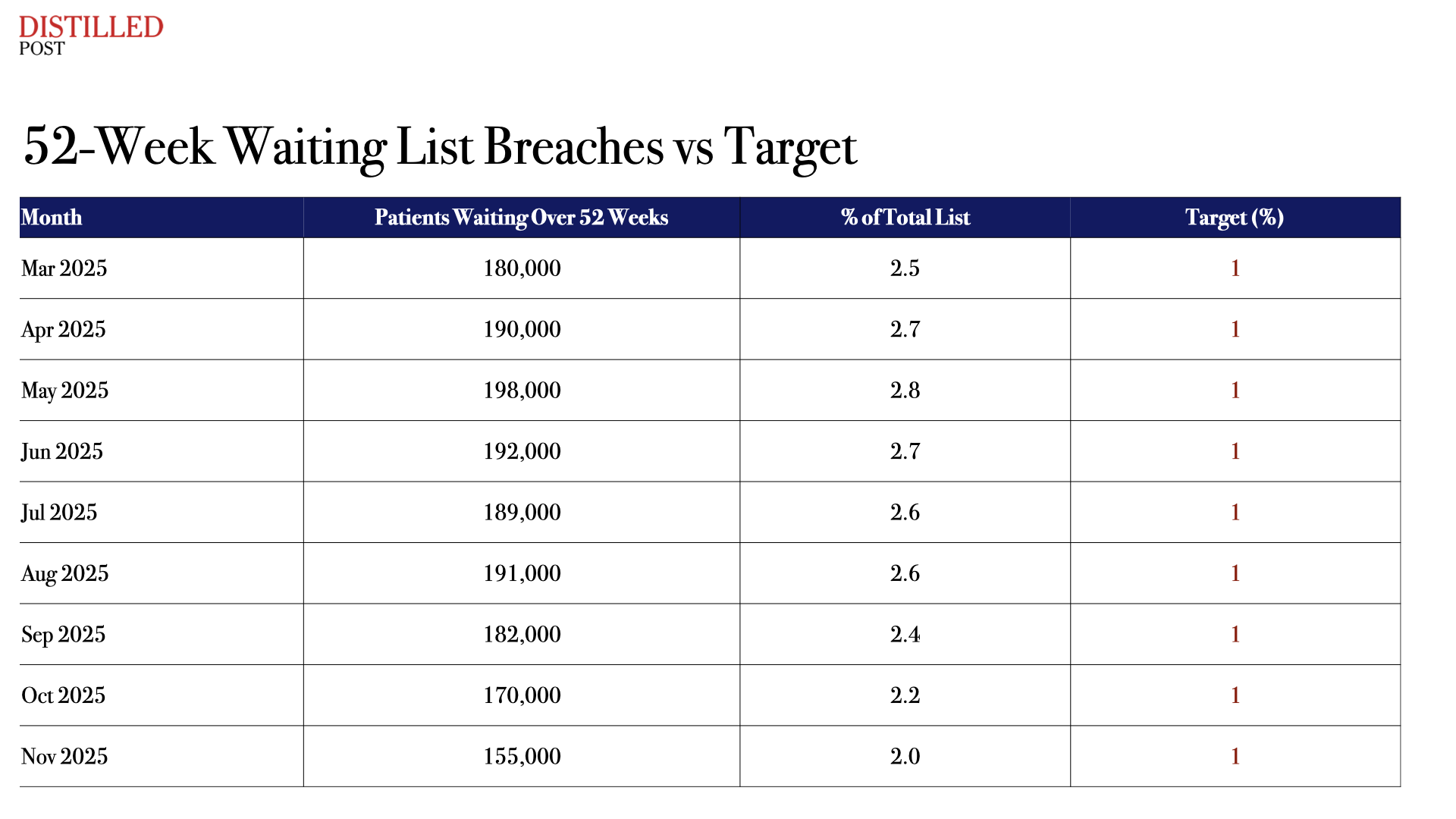
The strategic dilemma facing NHS England is therefore unavoidable. Delivering a visible improvement against the 18-week metric would represent a major political and operational milestone. It would signal that the NHS is regaining control over waiting lists after years of deterioration and disruption caused by the pandemic.
For Sir Jim Mackey and the national leadership team, the stakes extend far beyond a single performance indicator. Elective recovery sits at the heart of the broader government narrative about restoring NHS productivity and rebuilding public confidence in the health system. If waiting times begin to fall consistently, the NHS can argue that its recovery strategy is working.
However the longer-term challenge remains formidable. Even if the system reaches the 65 percent threshold this year, it remains far below the statutory standard that ultimately governs NHS performance. The long-standing national commitment is that 92 percent of patients should begin treatment within 18 weeks. Reaching that level would require a transformation in capacity and operational efficiency that extends far beyond short-term activity surges.
Delivering that transformation will demand expanded theatre capacity, major investment in diagnostics, improved workforce planning and more widespread adoption of digital tools that can streamline patient pathways. Without these structural reforms, the NHS risks repeating the cycle of short bursts of improvement followed by renewed stagnation.
The coming year will determine whether the current momentum represents the start of a genuine turnaround or simply a temporary surge designed to hit a symbolic target. For now, the numbers suggest the NHS may finally be approaching a turning point.
The real question is whether this sprint can evolve into a sustained recovery. Because once the headlines fade, the waiting list challenge will still remain.