

The NHS rarely gets credit when technology works. Yet across England, the Federated Data Platform (FDP) is beginning to deliver something the health service has struggled with for decades: visibility. While early implementation exposed gaps in data security compliance at some organisations, the response from NHS leaders has been pragmatic rather than punitive. Instead of ejecting trusts from the programme, the system has used the moment to strengthen governance, support improvement, and accelerate the benefits of a platform increasingly linked to better operational flow, performance and patient outcomes.
The initial challenge emerged during internal reviews of data security standards across hospitals connected to the FDP. Around a third of trusts using the system had not yet reached the minimum benchmark required by the NHS Data Security and Protection Toolkit. In most industries this might trigger immediate exclusion from shared platforms. The NHS took a different approach. Officials focused on remediation, providing targeted support to bring organisations into compliance while maintaining access to the operational insights the platform provides.
That decision reflects a broader strategic shift inside the health service. The FDP is not simply another IT project. It is the digital infrastructure behind a new operating model for hospital management, allowing clinicians, operational leaders and system managers to see the same real time data across waiting lists, bed capacity, diagnostic pathways and theatre utilisation.
The result is something the NHS has long lacked: a shared operational picture.
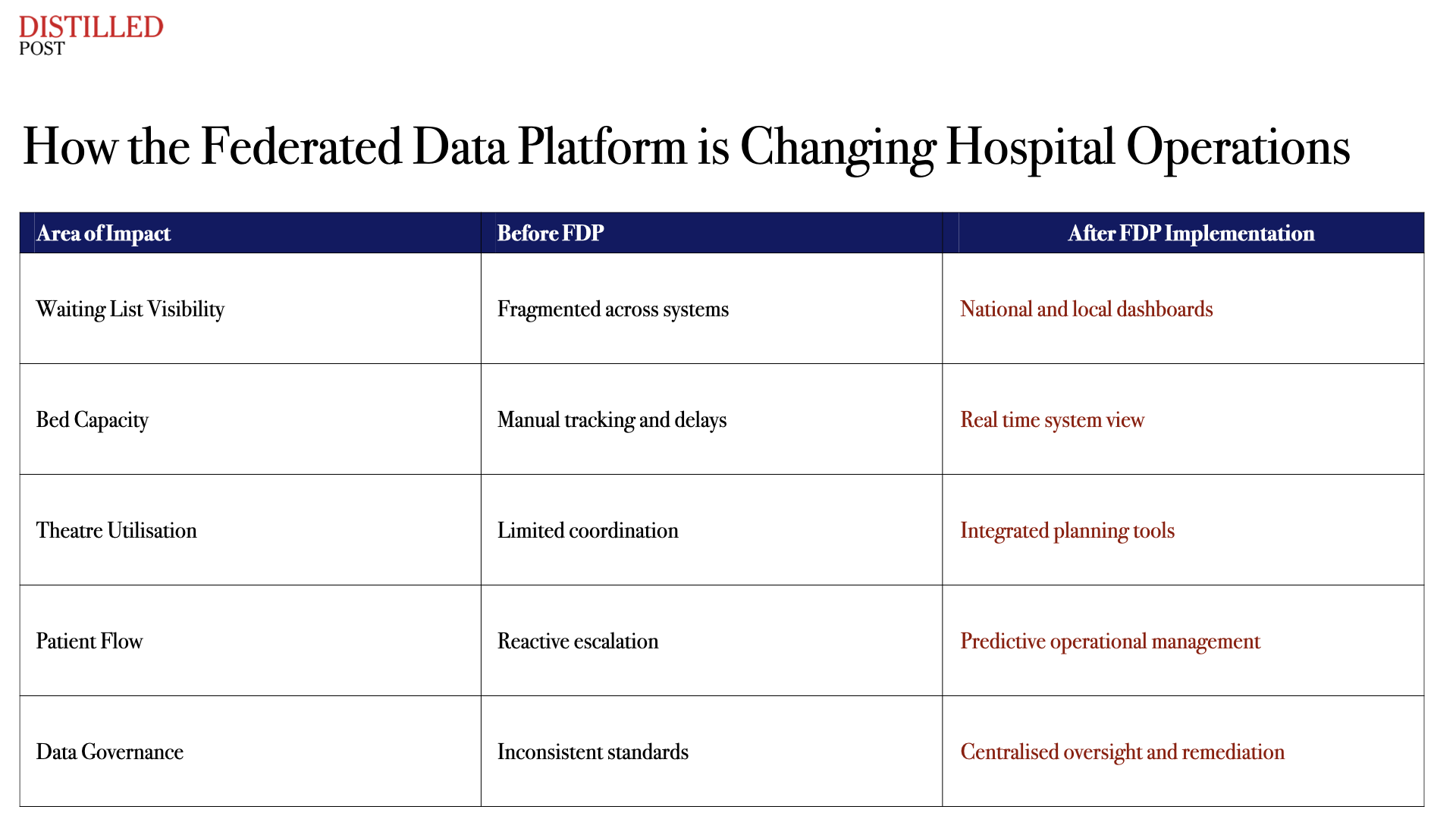
These changes matter because hospital performance rarely fails due to a single bottleneck. Delays cascade across departments: a blocked discharge slows emergency admissions, which stalls ambulance offloads, which then affects waiting times across the system. Without shared data, these problems often remain invisible until they become crises.
The FDP is designed to surface those pressures earlier.
The platform integrates operational data across multiple hospital systems and turns it into live dashboards used by clinical and operational teams. For executives running large trusts, it offers a system level view that previously required manual reconciliation of dozens of reports. For clinicians managing wards, it offers clearer insight into where patients are in the pathway and where delays are building.
More importantly, the platform allows different hospitals to operate with comparable information. That means regional teams and integrated care systems can coordinate activity rather than simply reacting to it.
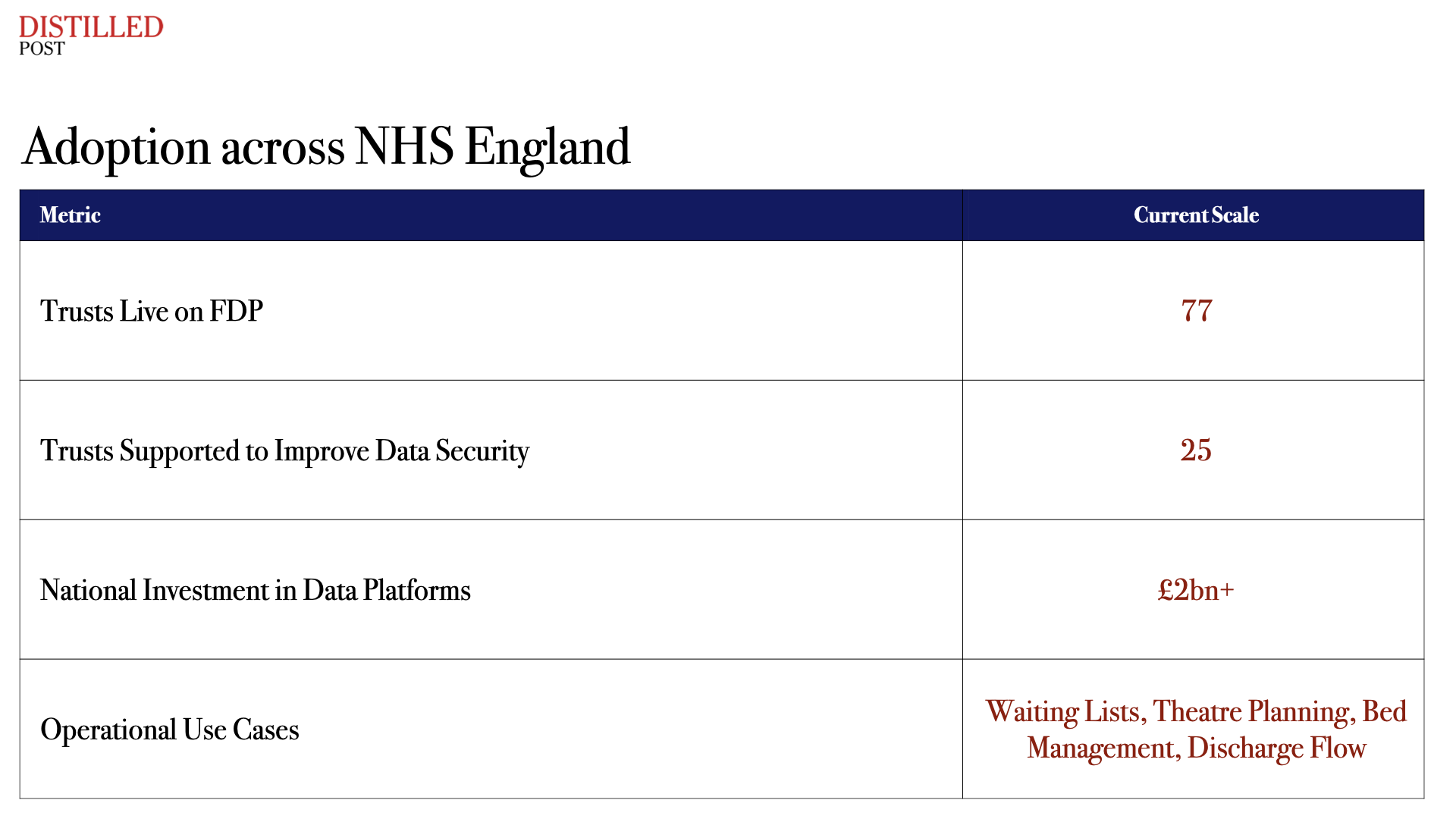
The early compliance gap identified during governance reviews was therefore less a failure of the platform and more a reflection of the NHS’s fragmented digital maturity. Many hospitals still operate with legacy infrastructure, and the transition to shared data systems inevitably exposes weaknesses that previously remained hidden.
In that sense the FDP is functioning as a forcing mechanism for improvement.
Rather than ignoring security weaknesses buried inside local systems, the platform has compelled trusts to strengthen governance and cyber resilience. NHS England has responded by offering direct support to organisations struggling to meet the required standards, ensuring the programme continues while risks are mitigated.
That approach is significant. Digital transformation programmes often fail when early problems trigger political backlash or institutional caution. Instead, NHS leaders have taken a more pragmatic stance: fix the issues, strengthen the controls, and keep moving.
What the Platform Is Delivering
The most tangible improvements are appearing in hospital operations. Several trusts using FDP tools report faster identification of delayed discharges and clearer tracking of diagnostic pathways. That visibility helps hospitals intervene earlier, reducing the number of patients stuck in beds while awaiting community care or follow up tests.
Operational leaders describe the platform less as a database and more as a “control tower” for hospital activity. By aggregating data from across departments, the system allows teams to spot pressure points before they escalate into full scale operational incidents.
That capability is particularly important during winter pressures, when hospitals must balance emergency demand with planned care.
The broader strategic goal is to move the NHS from reactive crisis management toward predictive system management. If hospital leaders can see pressure building days earlier, they can redirect resources, adjust theatre schedules or accelerate discharge planning before waiting lists or emergency departments become overwhelmed.
It is an approach borrowed from industries such as aviation and logistics, where real time operational oversight has long been standard.
Healthcare is only now catching up.
Criticism of the FDP has often focused on the politics of technology suppliers or the complexities of handling sensitive patient data. Those concerns are legitimate and have forced the NHS to strengthen governance frameworks. Yet they risk obscuring the bigger story unfolding across hospitals.
For the first time, the NHS is beginning to run parts of its hospital network on shared operational intelligence.
And that changes how decisions are made.
Instead of relying on fragmented local reports, leaders can see activity patterns across trusts, compare performance in real time and intervene earlier when services fall behind. Over time, that visibility could reshape how the health service manages waiting lists, allocates resources and responds to demand shocks.
The platform is still evolving and not every hospital has fully integrated its systems. But the trajectory is clear. As data quality improves and adoption spreads, the FDP is becoming less controversial technology and more essential infrastructure.
The NHS has spent years searching for tools capable of addressing its structural pressures: growing waiting lists, workforce shortages and rising demand. Technology alone cannot solve those problems. But it can give leaders the information they need to manage them.
The Federated Data Platform is beginning to do exactly that.
And quietly, across dozens of hospitals, it is helping the NHS see itself more clearly than ever before.