The NHS has halted two more major electronic patient record launches after national leaders raised concerns about operational disruption during one of the most pressured periods of the year for hospitals. The decision reflects a growing recognition that digital transformation must not undermine patient flow, elective recovery or data accuracy. Instead, NHS England is applying tighter oversight to ensure hospitals can adopt new systems safely while maintaining the operational stability required across emergency care, planned treatment and national performance reporting.
Digital Transformation Meets Operational Reality
Electronic patient records promise a modern, connected health service. In practice, their introduction often brings operational turbulence before the benefits are realised.
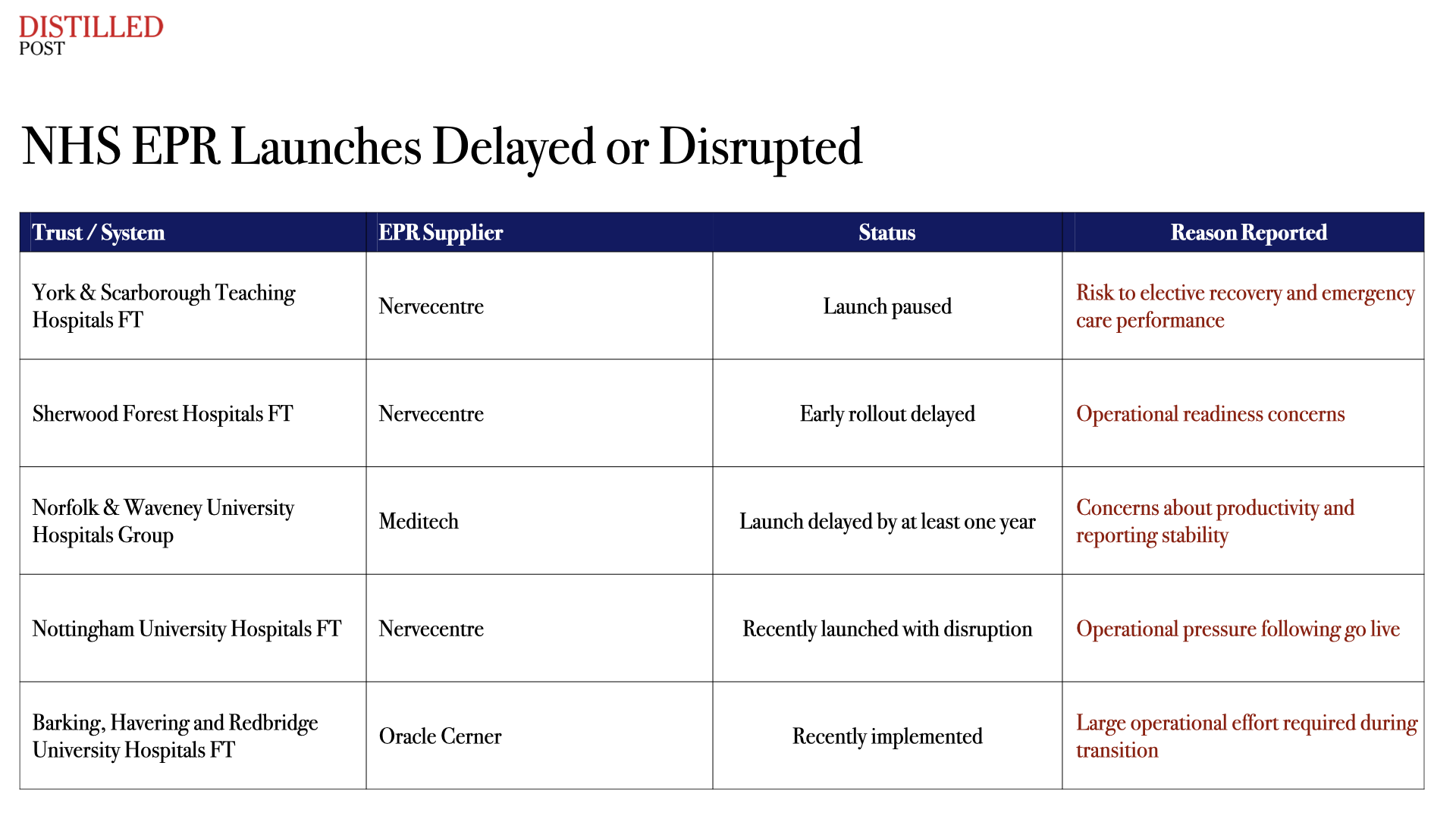
Two hospital groups preparing to activate new systems have now paused implementation after intervention from NHS England. Leaders feared that introducing the platforms at this moment could disrupt hospital activity, particularly elective surgery and emergency care, just weeks before critical national performance deadlines.
The intervention reflects a more cautious approach emerging at the centre of the NHS. Sir Jim Mackey has made clear that digital transformation cannot come at the expense of operational performance or patient safety. Trusts must demonstrate readiness, workforce training and operational stability before switching on complex clinical platforms that affect every part of hospital operations.
Behind the scenes, specialist national support teams are already working with trusts preparing to go live.
The Most Dangerous Moment in a Digital Programme
Electronic patient record launches represent one of the most complex operational changes a hospital can undertake. Thousands of staff must adapt to new workflows overnight while clinical documentation, prescribing, diagnostics and patient tracking move onto a new digital backbone.
When the transition works well the benefits can be transformative. Clinicians gain clearer visibility of patient histories, prescribing becomes safer, operational teams gain better oversight of patient flow and leadership teams benefit from stronger data.
But when implementation is rushed or poorly supported disruption can quickly ripple across the hospital.
Several trusts in recent years have experienced temporary slowdowns in theatre productivity, emergency department flow and outpatient activity following EPR launches. These impacts are rarely permanent, but they occur precisely when national performance targets leave little room for disruption.
Senior figures across the NHS say this is why a new approach is emerging. Rather than allowing trusts to push ahead independently, NHS England is applying tighter oversight before approving major digital launches.
Sources close to the programme say national tiger teams have been deployed to support sites preparing to go live. These teams combine operational, digital and clinical expertise to stress test readiness, review workforce preparation and ensure reporting systems remain stable before activation. The goal is simple. Digital transformation must improve hospitals, not destabilise them.
The Data Problem Few People Talk About
While operational disruption often dominates discussion, insiders say the deeper issue surrounding EPR launches lies in data integrity.
Hospital data underpins almost every national performance measure. Waiting list management, elective recovery, financial planning and regulatory oversight all depend on accurate and consistent reporting from local systems. If that data becomes unstable during a system transition, leaders can quickly lose visibility of patient pathways.
This challenge becomes particularly acute in the final quarter of the financial year when the NHS is attempting to demonstrate progress against waiting list and productivity targets. Accurate elective reporting depends on several critical data elements functioning perfectly. Referral pathways must migrate correctly. Waiting list clocks must remain intact. Theatre utilisation data must flow correctly into national reporting systems. Even short interruptions can create confusion for hospital leadership teams trying to validate activity levels or demonstrate performance improvement.
For NHS England the stakes are national. If hospital reporting becomes inconsistent, regional and national teams may struggle to assess whether recovery targets are genuinely being achieved. This explains why some launches have been paused.
Sir Jim Mackey has taken a pragmatic approach focused on managing risk rather than accelerating timelines. The priority is ensuring that hospitals retain operational visibility and data integrity during digital transitions.
That focus has also highlighted a structural issue in the digital ecosystem. Many EPR systems were originally designed around clinical documentation rather than alignment with national NHS reporting frameworks. Hospital leaders increasingly argue that suppliers must support operational flow management, waiting list validation and national performance reporting as core capabilities rather than afterthoughts.
In a system where data increasingly drives decision making, that alignment has become essential.
Suppliers Under Pressure to Support NHS Operations
The recent delays also shine a spotlight on the growing expectations placed on EPR suppliers.
Hospital leaders say many systems were originally designed around clinical record keeping rather than the operational complexity of running a large modern hospital. Today’s NHS relies on real time operational intelligence. Leaders must manage emergency department flow, elective waiting lists, theatre scheduling, workforce allocation and outpatient capacity simultaneously. If a new system fails to support these operational realities from day one the impact can be immediate.
Emergency departments slow down as staff adjust to unfamiliar workflows. Theatre productivity dips as digital scheduling tools are introduced. Reporting pipelines struggle while data definitions shift between legacy systems and new platforms.
Trusts usually recover from these issues over time, but the short term impact can be significant. That experience is changing how national leaders assess digital programmes.
Suppliers are increasingly being challenged to align their platforms with the NHS’s operational priorities. Systems must support elective pathway validation, national activity reporting and local patient flow management from the moment they go live.
Hospitals also expect stronger implementation support from vendors, including on-site teams capable of working alongside clinicians and operational managers throughout the transition.
Technology alone is no longer enough. Successful digital programmes depend on operational understanding.
The NHS still wants modern electronic records and the long term benefits remain clear. But hospitals want systems that improve productivity rather than temporarily suppress it. In a service treating millions of patients every week, the success of digital transformation will ultimately be measured not by software but by whether hospitals run better after the switch is turned on.
A More Mature Phase of NHS Digital Transformation
Digital transformation in the NHS is not slowing. It is becoming more disciplined.
Electronic patient records remain central to the future of the health service, offering safer prescribing, better clinical visibility and stronger analytics. But experience has taught national leaders that timing and operational readiness matter as much as technology.
Launching complex systems in the middle of winter pressures or during elective recovery targets introduces risks that can outweigh the immediate benefits. By applying tighter scrutiny, deploying specialist support teams and ensuring trusts are operationally ready before go live, NHS England is attempting to manage those risks rather than react to them.
The message from the centre is increasingly clear.
Digital transformation must strengthen patient care, improve productivity and deliver reliable data. If a programme cannot demonstrate those outcomes on day one, waiting a little longer is the responsible decision. For a health service of this scale, caution is not hesitation. It is leadership.