

Kettering General Hospital and University Hospitals of Northamptonshire were not short of demand. They were short of coordination. Patients were waiting in one part of the system while capacity sat underused in another. The issue was not effort or clinical capability. It was visibility. With the Federated Data Platform, that changed. What followed was a shift from isolated delivery to coordinated care across organisational boundaries.
Before FDP, pathways were largely managed within each trust. This created natural friction. Even when capacity existed elsewhere, patients often remained within local queues. Decisions were made in silos, with limited ability to view or act on system-wide demand. The result was predictable. Longer waits, uneven utilisation and avoidable delays.
The introduction of Shared Patient Tracking Lists through FDP fundamentally changed this dynamic. For the first time, teams could see demand and capacity across both organisations in real time. Patients were no longer bound to a single provider pathway. They could be identified, prioritised and moved based on where care could be delivered fastest.
The impact was immediate and measurable. More than 1,435 patients were transferred between the two trusts. On average, those patients were treated 38 days sooner. That is over a month of waiting time removed, not through additional funding or estate, but through better coordination.
This shift also reinforced local performance improvements. At Kettering, theatre utilisation increased by 10.46 percent, enabling more procedures to take place within existing capacity. Over 30,000 RTT pathway validations were completed, improving the accuracy of waiting lists and ensuring that clinical focus remained on patients who still required treatment. Discharge delays reduced by 8.79 percent, further improving flow across the hospital.
The value here is layered. At a local level, performance improves through better utilisation and cleaner data. At a system level, access improves through coordination. Together, these effects compound.
Before vs After: System Coordination in Practice
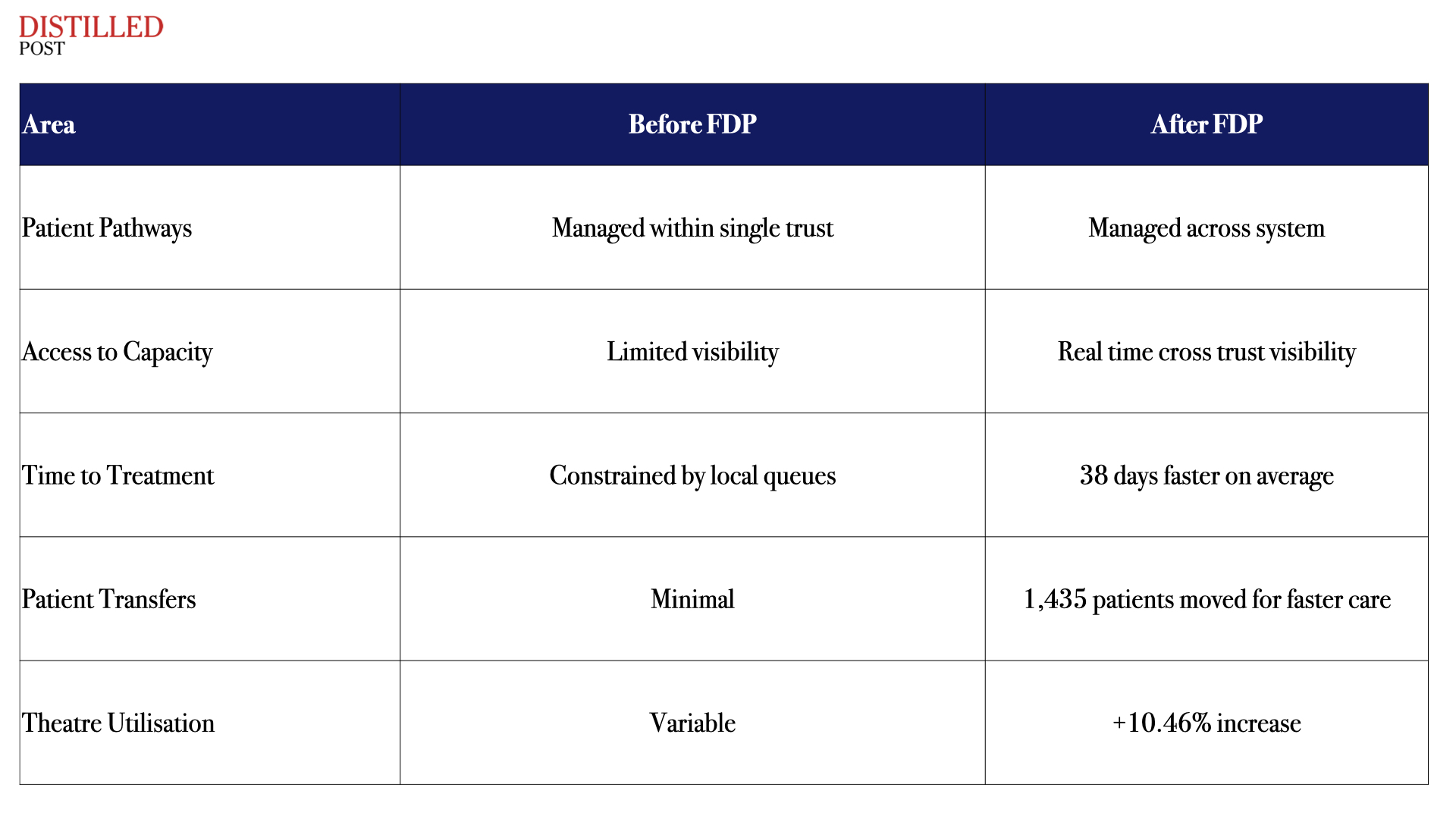
The broader implication is significant. This is no longer about improving a single hospital. It is about unlocking capacity across an entire system.
What Kettering and Northamptonshire demonstrate is that the NHS does not always need more infrastructure to treat more patients. It needs the ability to see and act across organisational boundaries. The FDP provides that capability. It turns fragmented capacity into coordinated delivery.

This is where the platform moves from operational improvement to structural change.
Patients are no longer constrained by geography. Capacity is no longer hidden. Decisions are no longer delayed.
Instead, the system begins to function as it was always intended. Connected, responsive and focused on delivering care as quickly as possible.
The result is simple. Faster treatment. Better use of resources. And a model that can scale far beyond a single region.