

It was never just about Palantir.
In Westminster this week, what should have been a focused examination of the NHS’s data infrastructure instead revealed something more familiar. A political dynamic taking hold, where attention shifts from systems to symbols, and from outcomes to actors.
At times, the debate resembled a kind of parliamentary theatre. Positions hardened quickly. Alliances formed along predictable lines. The identity of the supplier became the central point of contention, while the architecture it was tasked with delivering receded into the background. There was an air of something closer to a political tea-party, where the discussion was less about what is being built and more about who is allowed to build it.
That shift carries consequences. Because in focusing so heavily on Palantir as a company, Parliament risks overlooking the far more consequential question. Whether the NHS can function without the Federated Data Platform at all.
Across the debate, even the most critical voices acknowledged the same underlying reality. The NHS is fragmented. Data is dispersed across systems that do not speak to each other. Clinicians operate without a complete view of the patient. Operational leaders lack real-time visibility of flow, capacity and demand. The result is delay, duplication and inefficiency at scale.
The Federated Data Platform is designed to address that. Not as an abstract innovation, but as a practical response to structural failure. Even those raising objections accepted its potential. It could connect fragmented data across trusts, reduce discharge delays and cut cancer diagnosis times. These are not marginal gains. They go to the heart of how the NHS functions.
Yet those benefits have been pushed to the margins of the political conversation. In their place has come a more emotive debate about trust, ethics and the role of a single supplier. The result is a conflation that risks distorting the issue entirely.
To reject Palantir is not, in itself, a strategy for delivering a functioning data system.
Politics First, Policy Second
The tone of the debate is not occurring in isolation. It reflects a wider political climate in which positioning often precedes policy.
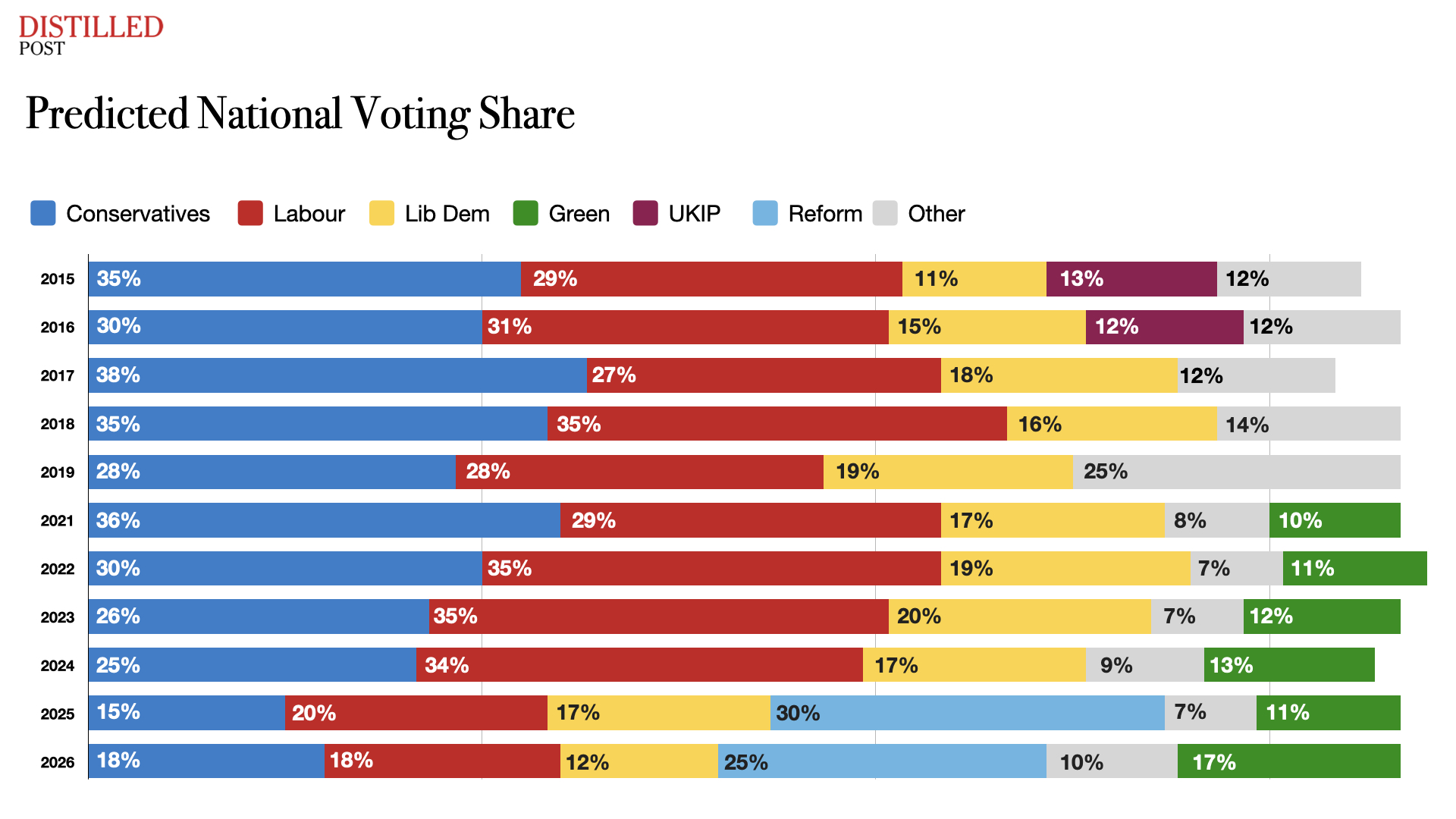
Recent polling shows a volatile electorate, with Labour’s lead narrowing, the Conservatives attempting recovery, and smaller parties such as the Liberal Democrats and Greens consolidating niche but vocal support bases. In that environment, issues like NHS data governance become proxies for broader ideological positioning.
For the Green Party, the argument is moral and absolute. Palantir represents a breach of NHS values and must be removed entirely. For the Liberal Democrats, the concern is structural, focused on lock-in, procurement and technical architecture. Labour’s position is more cautious, acknowledging both the potential of the FDP and the political risk attached to its delivery.
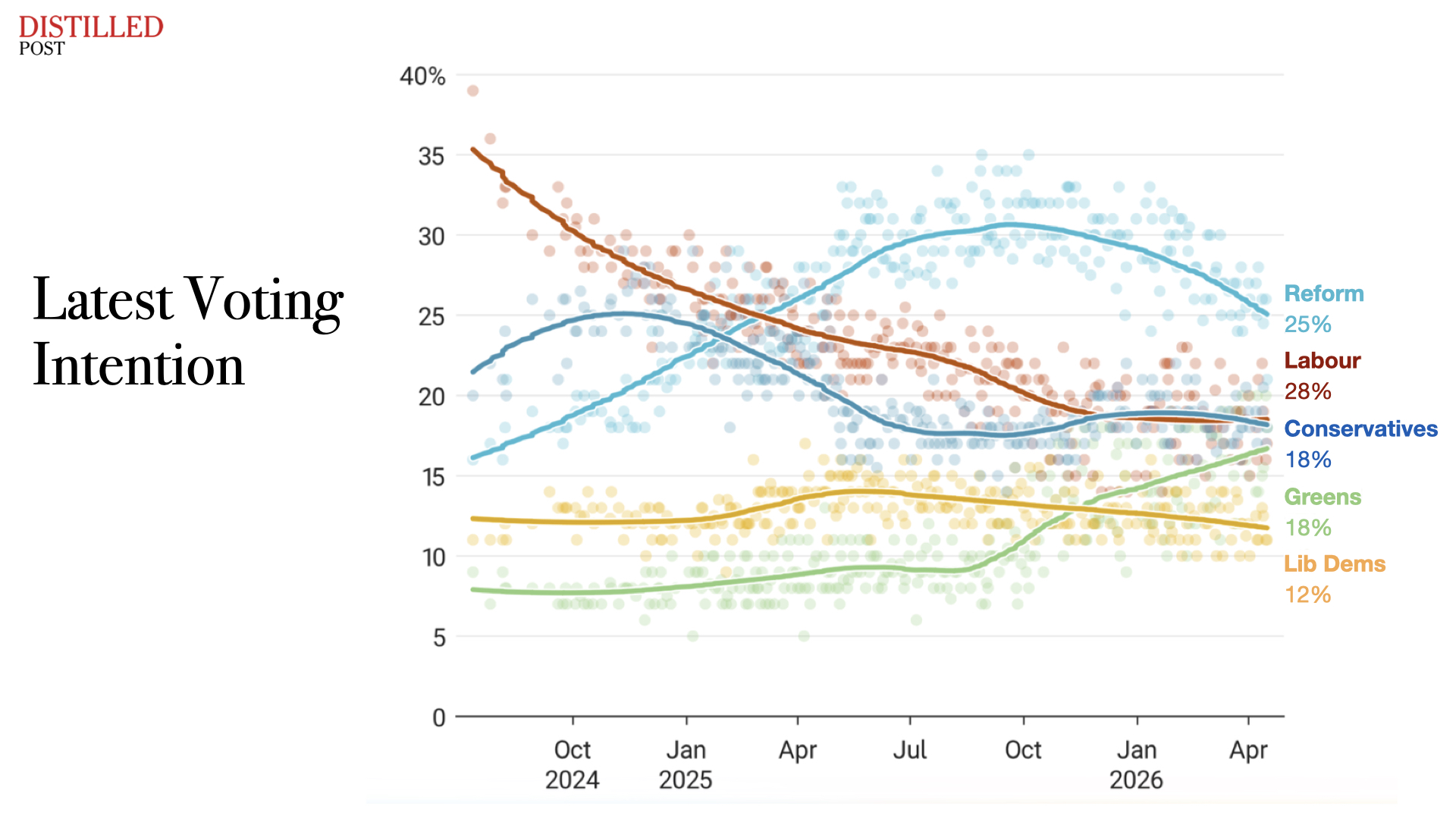
Each position reflects a constituency. Each carries internal logic. But taken together, they risk pulling the debate away from the system itself. Because the NHS does not operate in ideological fragments. It operates as a single, under-pressure system that requires coherence.
What are Ministers Saying
The sharpest criticism in the chamber was direct and, at times, visceral.
Samantha Niblett questioned whether Palantir could be “trusted as a custodian of the intimate health records of tens of millions of British citizens,” reflecting a broader unease about entrusting sensitive public data to a company whose leadership has openly criticised the NHS.
From the Liberal Democrats, the language became more forceful. One MP described the contract as “shameful” and warned that “Palantir… must have their hands ripped off of our NHS before it is too late.”
This was not a technical critique. It was a political and moral objection, rooted in distrust of the company’s wider associations and intentions.
The Green Party position went further still. Siân Berry argued unequivocally that “Palantir should be nowhere near our NHS data,” warning that public fear and loss of trust could become “catastrophic to health outcomes.”
Here, the argument moved beyond governance or procurement into a broader claim of incompatibility between the company and the founding principles of the NHS itself.
Other MPs focused on structure and sovereignty. Martin Wrigley warned of vendor lock-in and overdependence, arguing that Palantir represents a “single-point-of-failure” system that could embed itself across NHS infrastructure in ways that are difficult to reverse.
Yet even within this criticism, there was an important qualification. Few MPs disputed the need for the platform itself.
That distinction became clearer in the government’s response.
Dr Zubir Ahmed pushed back on the idea that the FDP is synonymous with a single supplier, stating plainly that “the FDP is fundamentally an NHS construct” involving multiple partners, and emphasising its role in improving efficiency and patient outcomes.
This more pragmatic line has also been echoed at senior levels. Health Secretary Wes Streeting acknowledged discomfort with the company’s politics, describing some of its leadership views as “pretty abominable,” while still defending the platform as “vital” to the NHS’s future.
Even Palantir itself has leaned into this distinction. Its UK leadership has insisted it has “no interest in patient data in the UK,” framing its role as purely infrastructural rather than custodial.
A System Designed for Another Era
The NHS today is not short of data. It is overwhelmed by it.
Across hospitals, GP practices, community services and specialist centres, vast quantities of information are generated every day. But that data remains fragmented, siloed and often inaccessible at the point of care. Clinicians frequently operate without a complete picture of the patient in front of them. Operational leaders struggle to understand flow, capacity and demand in real time.
This is not a marginal inefficiency. It is a structural limitation. Delays in discharge, missed diagnostic windows, duplication of tests, and inefficient allocation of resources all stem, in part, from an inability to connect information across the system. It is precisely this problem that the Federated Data Platform is designed to address. The government’s position during the debate reflected this reality. Ministers emphasised that modern care is not possible without data and its effective use.
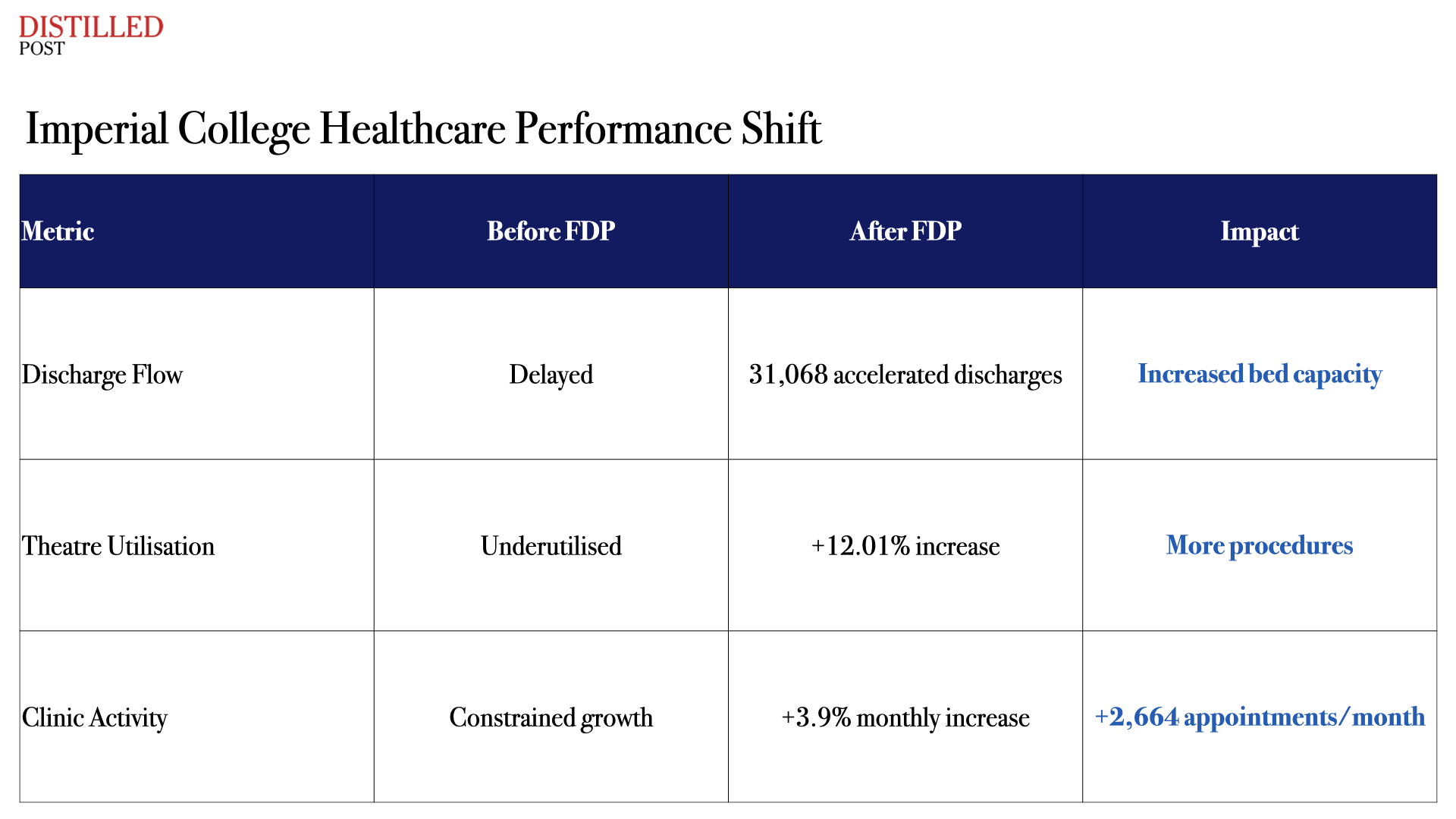
This is not a defence of Palantir. It is a statement about the system itself.
The Palantir Problem
Criticism of Palantir has been sharp and, in many cases, justified. Concerns raised in Parliament fall into several clear categories.
There are questions of trust, with MPs warning that public confidence in the NHS could be undermined if patients believe their data is being handled by a company whose values they do not share. There are concerns about sovereignty, particularly the reliance on a US-based firm for critical national infrastructure. There are challenges around procurement and governance, including the transparency of the contract and the long-term cost implications. There are technical concerns, including the risk of vendor lock-in and the embedding of proprietary systems across NHS trusts. And there are broader ethical objections, with some MPs citing the company’s global activities as incompatible with NHS principles. These arguments are not trivial. They demand response. But they do not negate the underlying need for the FDP.
Separating Platform from Provider
One of the most important distinctions to emerge from the debate is the difference between the FDP as a concept and Palantir as a supplier.
Too often, these have been conflated.
The FDP is an architecture. It is a framework for connecting data across disparate systems while maintaining local control. It is an attempt to create a coherent view of patient pathways and system performance. Palantir is a contractor delivering components of that architecture.That distinction matters because it reframes the question.
The issue is not whether the NHS should have a federated data platform. It is whether the current implementation, governance and supplier model are optimal. Those are questions that can be addressed without abandoning the programme altogether.
The Cost of Inaction
What has been less clearly articulated in the debate is the cost of doing nothing. These are not abstract metrics. They translate directly into patient outcomes.
Without integrated data, the system cannot, manage elective recovery effectively, identify patients at risk earlier, optimise use of limited clinical capacity or deliver coordinated care across settings. The FDP is not a silver bullet. But without it, many of these challenges become materially harder to address.
What the Debate Gets Right
Parliament has surfaced real and important concerns. Trust matters. Without public confidence, no data system can function effectively.
Governance matters. Large-scale technology programmes require transparency, accountability and oversight. Sovereignty matters. In a more uncertain geopolitical environment, the question of who controls critical infrastructure is no longer theoretical.
These are the right questions. But they must be held alongside an equally important truth.
What is missing from the debate is a sense of collective responsibility. It is true that the current government inherited the contract. It is true that opposition parties did not design the procurement. But the NHS cannot be rebuilt from first principles every electoral cycle.
Infrastructure of this scale demands continuity. Responsibility, in this case, is shared. If the FDP is to succeed, it will require a degree of political alignment that has so far been absent. Not unanimity, but maturity. A recognition that while vendors may change, the need for a functioning data system does not.
To reduce the conversation to Palantir is to narrow the field of vision at precisely the moment it needs to widen.
Beyond Palantir
In time, the specific supplier delivering the FDP may change. Contracts may evolve. New technologies will emerge. What should not change is the recognition that the NHS requires a coherent data infrastructure. The debate has, perhaps unintentionally, clarified that point. Even the strongest critics have acknowledged the need for better data integration. Even the most cautious voices have accepted that the status quo is unsustainable. This is a rare moment of underlying consensus.
The argument over Palantir has exposed something deeper than a disagreement about a single contract or supplier. It has revealed a system that is still uncertain about how to reconcile its founding principles with the realities of modern infrastructure, where data is no longer an administrative by-product but the foundation upon which care itself is delivered. That tension is understandable, but it cannot become paralysing.
The NHS stands at a point where incremental change is no longer sufficient. The pressures it faces are structural, persistent and increasingly complex, and they cannot be addressed through isolated interventions or fragmented improvements. They require a level of coordination, visibility and responsiveness that is simply not possible without a coherent data architecture operating across the system as a whole.
The Federated Data Platform represents an attempt, imperfect but necessary, to build that architecture. It is not without risk, and it is not beyond criticism, but it reflects a recognition that the status quo is no longer viable. To reject it outright is not to preserve the NHS as it is, but to accept a continuation of the inefficiencies and delays that already undermine patient care on a daily basis.
What is required now is not a retreat from the ambition of the FDP, but a more disciplined approach to its delivery. That means strengthening governance, ensuring transparency, and building public confidence through clear accountability and visible safeguards. It also means maintaining the flexibility to evolve the supplier landscape over time, reducing dependency where necessary while preserving the integrity of the system itself.