

The conversation around the NHS Federated Data Platform has become distracted. This is not, at its core, a debate about a single vendor. It is a test of whether the NHS is ready to operate as a modern, data-driven health system. The signals are already clear. The platform is live across the vast majority of the estate, delivering measurable improvements in productivity, patient flow, and clinical decision-making. The real risk now is not adoption. It is losing momentum.
The NHS has spent decades operating within fragmented systems. Data has been locked in silos across trusts, departments, and legacy platforms that do not communicate effectively. Clinicians and operational teams have compensated for this with experience and workarounds, but the cost has been visible: delays, inefficiencies, and inconsistent outcomes. The Federated Data Platform is a structural correction to that problem, creating a connected layer that allows the system to function as one.
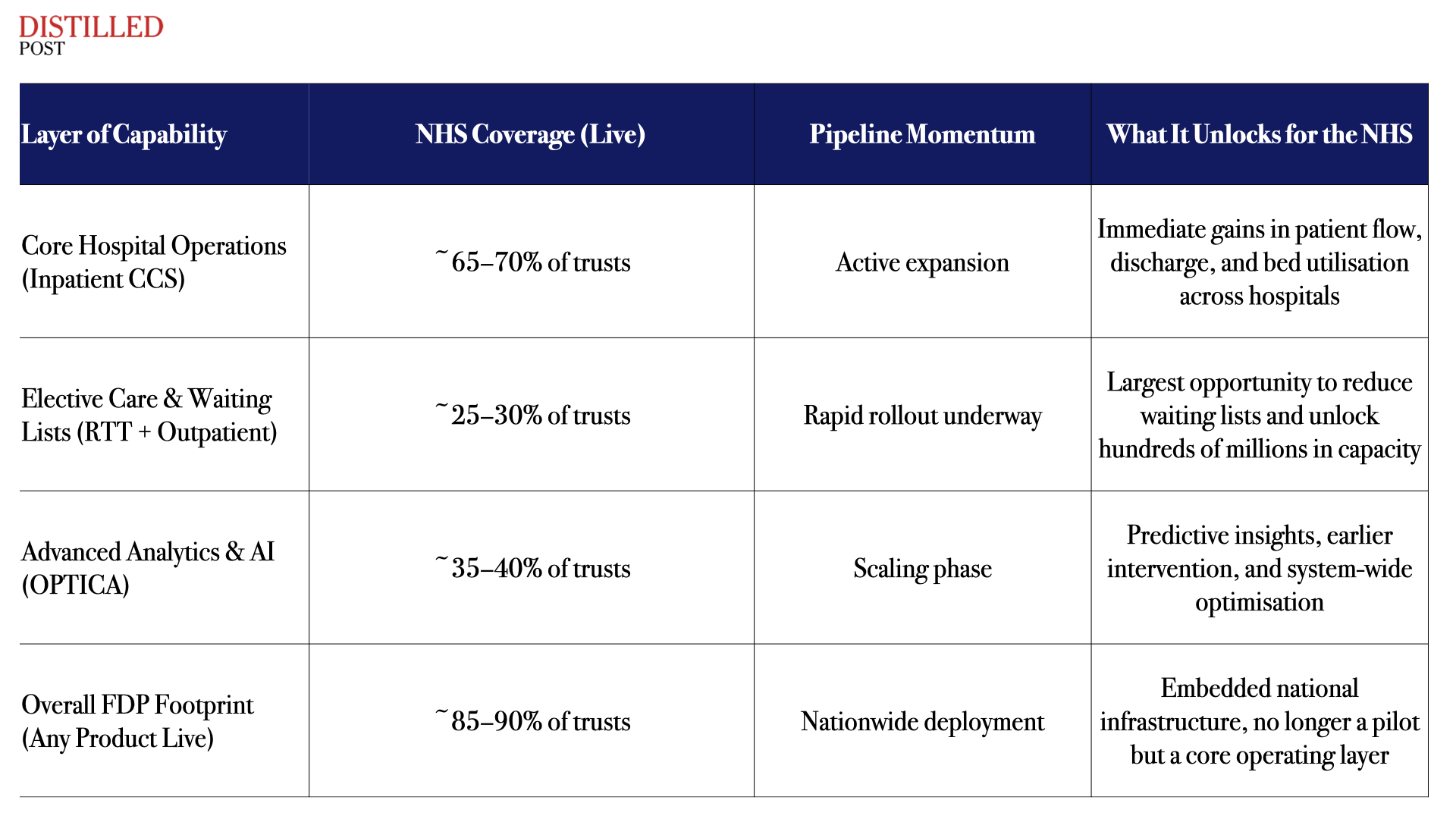
The rollout tells a very specific story. Core hospital operations are already live across roughly 65–70% of trusts. This is where the NHS has started, and for good reason. Patient flow, discharge management, and bed utilisation are the pressure points that define performance. Improvements here translate immediately into better outcomes and more efficient use of capacity. Hospitals move patients faster. Beds become available sooner. Decisions are made with clarity rather than guesswork.
The next phase is already underway. Elective care and outpatient pathways, where only around 25–30% of trusts are currently live, are now moving into rapid rollout. This is the layer that directly addresses waiting lists and backlog recovery. It is also where the financial impact becomes significant. Even a 1–2% improvement in productivity at this level can release £150m to £300m or more in capacity, before accounting for the wider benefits of earlier intervention and reduced complexity of care.
Above this sits the analytics and AI layer. Around 35–40% of trusts are now live or scaling advanced capabilities, moving the NHS from reactive operations to predictive management. This is where the system begins to anticipate demand, identify risk earlier, and allocate resources more intelligently. It is not yet universal, but it is expanding on top of a foundation that is already in place.
Taken together, the overall footprint is what matters. With 85–90% of trusts live on at least one component, the Federated Data Platform is no longer a pilot or a concept. It is becoming a core operating layer of the NHS.
At the top end of the system, the direction is just as clear. The Shelford Group, a coalition of the NHS’s ten largest and most research-intensive teaching hospital trusts, represents the leading edge of clinical complexity, innovation, and national service delivery. These organisations collectively shape standards, influence policy, and manage some of the most demanding patient pathways in the country.
Around 60% of Shelford Group hospitals are already using or actively rolling out the Federated Data Platform. These are not early adopters in the traditional sense. They are the most sophisticated environments in the NHS, balancing acute care, research programmes, and system-wide responsibilities.
Trusts such as Manchester University NHS Foundation Trust, Imperial College Healthcare NHS Trust and The Newcastle upon Tyne Hospitals NHS Foundation Trust are already using the platform to support operational flow and system performance at scale. Others, including Cambridge University Hospitals NHS Foundation Trust, are sequencing adoption alongside major electronic patient record deployments, with plans to expand into analytics, complex discharge, and research-aligned use cases.
The remaining group, largely those stabilising new EPR environments, are not rejecting the platform. They are delaying. Their roadmaps already include future rollout aligned to broader transformation programmes and research objectives. In practical terms, this means the majority of the NHS’s most advanced hospitals are either already using the platform or preparing to.
This is what real system transformation looks like. Not a single moment of adoption, but a staged build. First, stabilise core operations. Then unlock elective capacity. Then optimise the system through data and AI. The NHS is partway through that journey, with the most valuable gains still ahead.
The key point is simple. The Federated Data Platform is already delivering where it is live. It is expanding rapidly into the areas that matter most. And at the highest level of the NHS, adoption is no longer a question of if, but when.
The priority now is not to revisit the decision. It is to execute, scale, and realise the full value of what is already in motion.